As ICE enforcement intensified in Minnesota, Minneapolis residents built a parallel healthcare network of volunteer clinics and rotating locations. Now other cities are asking whether they should do the same — and what it means when a shadow medical system becomes necessary.
Minneapolis has seen the development of a notable public health response: a network of volunteer-run, underground health clinics created in direct response to intensified ICE enforcement operations across Minnesota.
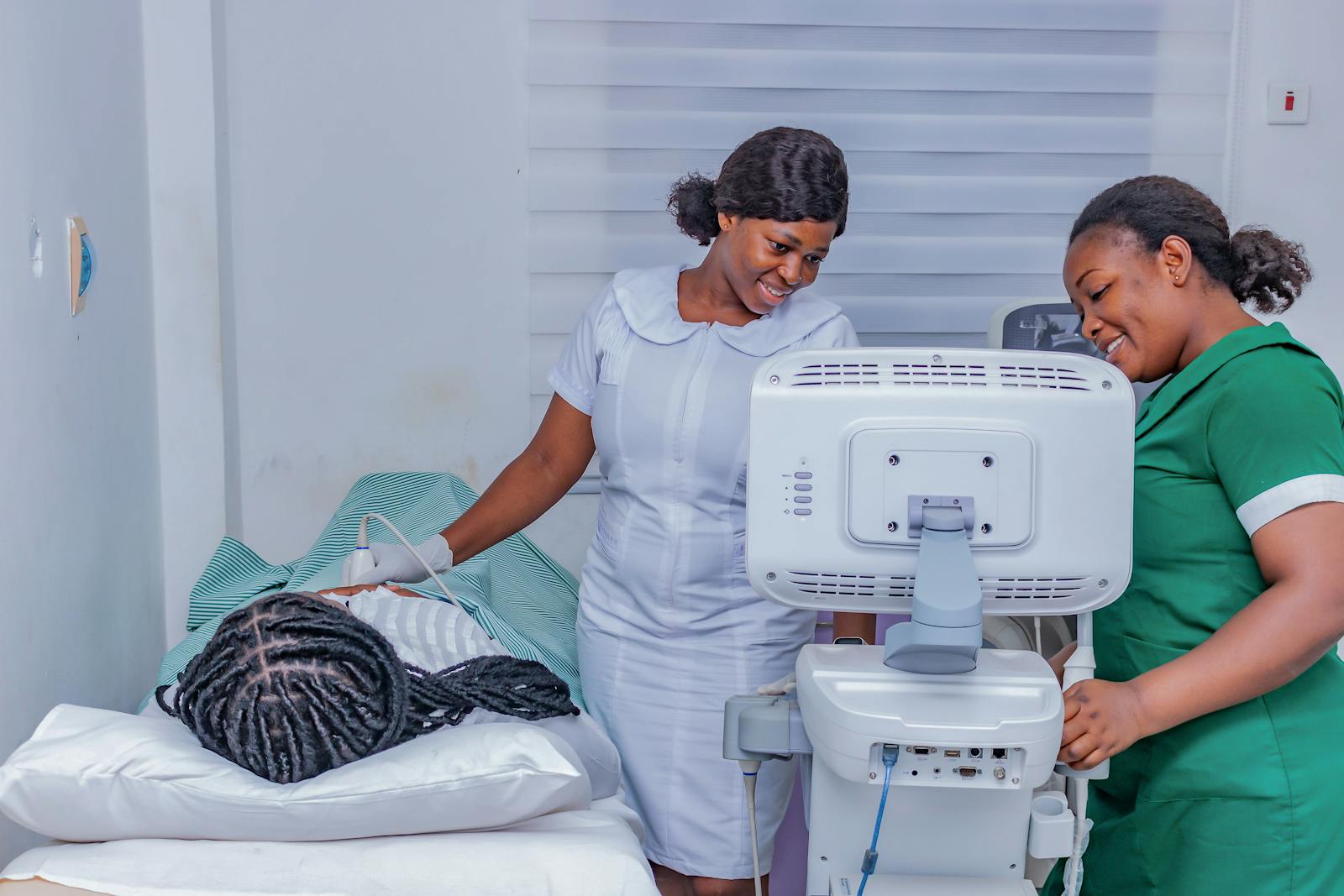
As immigration enforcement surged in the Twin Cities region, immigrant families began avoiding hospitals, clinics, and pharmacies out of fear. The result was a widening gap in basic healthcare access — and a grassroots response that's now drawing attention from communities across the country.
The question gaining traction: should other cities replicate what Minneapolis built?
How Fear Reshaped Healthcare in the Twin Cities
The pattern was consistent. As ICE operations expanded in Minnesota — with reports of increased agent presence at one point — undocumented residents and mixed-status families began pulling back from the formal healthcare system. Routine checkups stopped. Prescriptions went unfilled. Parents delayed bringing sick children to emergency rooms.
These fears were reportedly grounded in real enforcement concerns. Reports indicated that families afraid of ICE were actively forgoing medical care, with volunteers stepping in to fill the vacuum. The chilling effect extended beyond undocumented individuals — legal residents in immigrant-heavy neighborhoods also reported anxiety about visiting healthcare facilities.
The downstream consequences ripple outward in ways that affect everyone, not just immigrant communities. Untreated infections spread. Unmanaged chronic conditions become emergencies. Preventive care vanishes. The entire public health infrastructure starts to buckle under pressure it wasn't designed to absorb.
A Shadow Medical System Takes Shape
Minneapolis didn't wait for a policy fix. Instead, a loose coalition of healthcare workers, community organizers, and volunteers assembled what has been described as a "shadow medical system" — a parallel healthcare network operating outside traditional institutions.

These networks look different from a standard free clinic. Locations rotate. Communication happens through encrypted channels and trusted community contacts. Volunteers include off-duty nurses, retired physicians, medical students, and community health workers who speak the languages of the populations they serve. The focus is practical: blood pressure checks, wound care, medication management, prenatal screenings, and connecting people to resources they can access safely.
The model borrows from mutual aid traditions that have roots in communities of color and immigrant neighborhoods. Think less "rogue hospital" and more "neighbors with medical training making house calls."
What makes the Minneapolis approach notable is its scale and coordination. This isn't one church basement with a volunteer nurse. It's a networked response across multiple neighborhoods, organized enough to function reliably but decentralized enough to avoid becoming a target.
The Nutrition Connection
Healthcare access and food access are deeply intertwined, and the Minneapolis situation highlights both. When families avoid public-facing institutions, they often pull back from food assistance programs, community kitchens, and grocery stores in heavily patrolled areas.
Nutrition becomes a casualty of fear. Families stockpile shelf-stable, calorie-dense processed food instead of making regular trips for fresh produce. Dietary management for conditions like diabetes or hypertension — already disproportionately affecting communities of color — falls apart when people can't see a doctor or safely access a grocery store.
Some Midwest communities have community-centered food spaces, including Black-owned vegan restaurants that can serve as cultural gathering points and nutritional anchors for their neighborhoods. When the surrounding community contracts under fear, those businesses and the food ecosystems they support feel the pressure too.
Some of the Minneapolis volunteer networks have incorporated food distribution into their health outreach — delivering fresh fruits, vegetables, and culturally appropriate meals alongside medical supplies. The logic is straightforward: you can't address someone's health without addressing what they eat.
Should Other Cities Follow?
The question is central, and the answer is more complicated than it might seem.
On one hand, the Minneapolis model demonstrates what community self-organization can accomplish when institutional systems become inaccessible. It's responsive, culturally informed, and built on trust. Those are qualities that formal healthcare systems spend years and millions of dollars trying to cultivate.
On the other hand, underground health networks exist because the above-ground ones failed a population. That's a structural problem, not a feel-good community story. Volunteer clinics can't perform surgeries. They can't run MRIs. They can't manage complex cancer treatment protocols. The ceiling on what informal networks can provide is real, and people will suffer at that ceiling.

There's also the question of sustainability. Volunteer energy is finite. Burnout is real — something research on energy management demonstrates. A shadow medical system that depends on the goodwill and spare time of healthcare professionals has an expiration date unless it evolves into something more sustainable.
Cities watching Minneapolis are reportedly weighing their options. The playbook isn't secret: identify trusted community connectors, recruit medical volunteers, establish secure communication networks, partner with faith organizations and cultural institutions, and build redundancy so no single point of failure brings the whole thing down.
The Broader Economic Picture
Healthcare isn't the only system feeling the impact. Measuring the full economic damage of Minnesota's ICE surge has proven difficult, but the effects are visible: businesses in immigrant-heavy neighborhoods have seen foot traffic decline, workers have pulled back from jobs, and the ripple effects touch industries from food service to construction to agriculture.
When people stop moving freely through a city, the city's metabolism slows. Restaurants lose customers. Markets lose vendors. The interconnected web of small businesses, cultural institutions, and community organizations that makes urban neighborhoods functional starts to fray.
The claims and counter-claims around enforcement numbers have themselves become a source of confusion, with numerous reports investigating various claims about Minnesota's immigration crackdown, reflecting the fog of misinformation that surrounds the situation and compounds the fear driving people away from public life.
What This Means for the Rest of Us
Here's the thing that makes this a story about more than immigration policy: the health of a community is not divisible. You can't carve out one population's access to healthcare and expect the broader public health picture to stay intact.
Unvaccinated children spread disease to all children. Untreated tuberculosis doesn't check immigration status. A pregnant woman who can't get prenatal care becomes a far more expensive emergency patient when complications arise — and that cost gets absorbed by the same hospital system everyone uses.
The Minneapolis underground health networks are, in one sense, a testament to human resourcefulness and solidarity. People saw a gap and filled it with whatever they had. That impulse — the instinct to feed, heal, and protect the people around you — is about as fundamental as it gets.

But they're also a warning signal. When a major American city needs a parallel healthcare system to serve residents who are too afraid to use the official one, something has gone sideways at a systemic level.
Other cities are watching. Some are already building. The model Minneapolis created wasn't designed to be permanent. Whether it becomes a template or a cautionary tale depends on what happens next — both in Minnesota and in the halls of policy far from the church basements and living rooms where volunteers are checking blood pressure and handing out fresh vegetables.
The underground networks will keep running for as long as they're needed. The better question might be: how do we build a world where they're not?
Feature image by RDNE Stock project on Pexels















